Revision bariatric surgery
A number of patients who have undergone weight loss surgical procedures in the past are now seeking revision surgery for complications of the previous procedure or weight regain.
Revision bariatric surgery requires careful planning and should only be performed by experienced surgeons in large institutions that have the expertise required to undertake all the essential pre-operative tests and look after these patients during and after surgery. These are highly complex operations due to the scar tissue from the previous surgery and unless they are performed carefully, they can be associated with a high risk of complications.
Mr Moorthy routinely performs revision bariatric surgery with excellent results and is supported by a team of endoscopy and radiology specialists, bariatric and endocrine physicians, dietitians and psychologists. He performs these operations in the Wellington hospital and Lindo Wing of St Mary's Hospital as these hospitals have all the necessary facilities to carry out these complex laparoscopic operations. Both these facilities also offer the possibility of undertaking these operations with the use of the robot which make stitching, as essential aspect of these operations, safer.
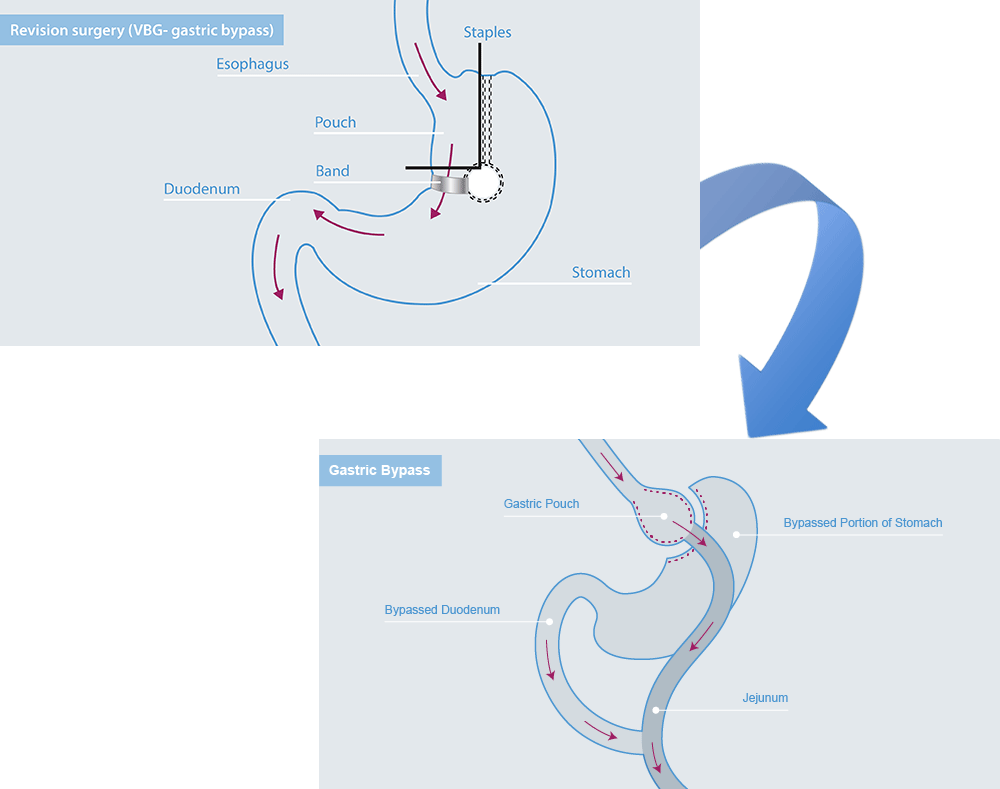
Previous vertical banded gastroplasty
A number of patients, especially from the Middle East, who have undergone this operation are now suffering from complications. The problems associated with this operation and now well recognized and this operation is no longer accepted as a safe and effective bariatric procedure.
Patients experience vomiting, difficulty in swallowing and severe acid reflux due to the severe narrowing of the stomach pouch as a result of this operation.
The only approach to help these patients is to perform a Roux-en-Y gastric bypass.
Previous gastric band
A number of patients with gastric band are experiencing complications such as vomiting, acid reflux, difficulty swallowing or band slippage. Emptying the band does not help as the band is often surrounded by a capsule of scar tissue which causes a tight blockage even if the band is emptied.
Following the removal of the gastric band, patients can either be converted to a sleeve gastrectomy or a gastric bypass. Generally, it is considered to be good practice to remove the band first and then perform a second operation 6-8 weeks later to give some time for the scar tissue to soften. This is especially important in patients who want a sleeve gastrectomy as the second procedure as the risk of a leak is four times higher in revision surgery as compared to primary (first time) surgery. However, if the patient desires a gastric bypass, this can be done at the time of the gastric band removal.
Previous sleeve gastrectomy
Usually the need to convert a sleeve gastrectomy to a gastric bypass is rare unless the original operation has not been performed well or there are complications such as acid reflux and difficulty swallowing. A poorly performed sleeve either results in insufficient weight loss or a risk of weight regain.
If done well, conversion of the sleeve gastrectomy to a gastric bypass is not associated with a high risk of complications and good results. The principle is to convert the gastric sleeve to a small stomach pouch by stapling across the sleeve and then performing a gastric bypass.
Previous gastric bypass
The reasons for revision surgery maybe due to insufficient weight loss, weight regain or complications such as non-healing ulcers.
Failure to lose weight or weight regain may have a number of causes, which need to be clarified before considering further surgery. It is essential that patients are seen by a dietitian and a psychologist prior to consideration of revision surgery.
There are various strategies for revision surgery in patients who have had gastric bypass- inserting a band over the gastric pouch, shortening the gastric pouch, revising the join between the pouch and the intestine and lengthening the alimentary limb. The appropriate strategy is determined by undertaking a detailed consultation with the patient and after investigations that may involve an endoscopy and barium studies.